The New York Health Care Reform Act of 2000 (HCRA 2000), signed into law at the end of 1999, creates a new framework for health care finance in New York State. By extending and expanding legislation enacted in 1996, HCRA 2000 addresses a broad range of issues, including mechanisms for hospital reimbursement, graduate medical education finance, and subsidies for care provided to the uninsured. The new legislation enacts a number of major changes to increase funding for health care and attempts to increase access to health insurance.HCRA 2000 programs are expected to cost a total of $8.7 billion over the next three and a half years. Nearly $2.8 billion will come from two new funding sources: an increase in the cigarette tax of 55 cents per pack ($1.5 billion) and state collections from the tobacco litigation settlement ($1.3 billion). Prior to HCRA 2000, most of the tobacco settlement funds were to be used for state debt reduction. The remaining $5.9 billion will come from existing funding streams. These include a payment that hospitals must make representing 1.0 percent of their revenues, an assessment on managed care plans for each member covered, and an 8.18 percent tax on all hospital payments made by health care insurers.
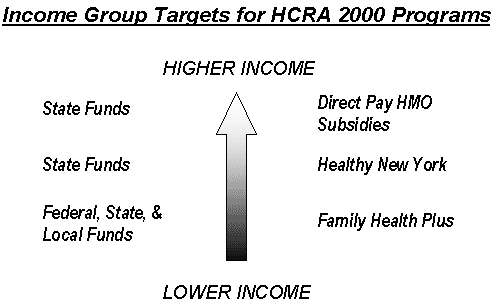
Expanding Access to Health Care. A centerpiece of the HCRA 2000 legislation is the creation of several new programs that will increase the number of people who have access to health care insurance. This is especially relevant for New York City when almost one in five city residents under 65 are uninsured. In addition to continuing to fund Child Health Plus-a program created in 1996 to provide health insurance to children whose parents could not afford to pay for it-HCRA 2000 attempts to extend the availability of insurance by establishing several new programs to make insurance more affordable. The new programs target three different income groups: low-income, low- to moderate-income, and moderate-income and above. These programs will be funded primarily by state revenues set aside for HCRA 2000. However, Family Health Plus (the low-income program) will also be partially funded by local governments, including New York City.
Family Health Plus: Low-Income. Family Health Plus is a fully subsidized health insurance program targeted to the adult population that is not currently eligible for Medicaid. Those who choose to enroll will sign up with a participating managed care plan to receive services. Adults in families with children will be eligible to enroll if their total family income is less than 150 percent of the Federal Poverty Level (FPL)-$25,000 for a family of four. Single adults without children will qualify if their incomes are less than 100 percent of the FPL-approximately $8,300. Family Health Plus will largely be funded by Medicaid, the costs of which are shared by New York City, New York State, and the federal government.
The fiscal impact of Family Health Plus on New York City will be determined by how many people enroll and how much each person will cost. Estimates derived from recent census data indicate that there are between 300,000 and 350,000 adults eligible for Family Health Plus in New York City. Assuming between 40 and 50 percent enroll, we expect that approximately 150,000 adults would sign up when the program is fully implemented. Premium rates to be approved by the NYS Insurance Department are likely to fall between $200 and $250 per enrollee per month. The city's share of those expenses would be 25 percent. If the program becomes operational in the summer of 2001, and grows at 3,000 enrollees a month the first year and slightly faster for the next two years, the cost to the city through the summer of 2004 could approach $125 million - $15 million the first full year, $40 million the second full year, and $70 million the last year.
There is a possibility, however, that Family Health Plus will not have any fiscal impact on New York City. The State Senate and Assembly both favor legislation that would eliminate local government responsibility for paying a share of program expenses. If this legislation is signed into law the state would pay the full non-federal amount. This issue is expected to be included in the current round of New York State budget deliberations.
Healthy New York: Low- to-Moderate Income. HCRA 2000 also establishes a program called Healthy New York that is targeted at small businesses that cannot afford to provide health insurance for all their employees. It creates a new managed care option that will be available only to those businesses or individuals that meet the eligibility requirements. HCRA sets aside funds to provide HMOs up to 90 percent of the expenses for any individuals whose care costs between $20,000 and $100,000 per year. These HCRA subsidies will allow HMOs to reduce their premiums, which in turn will make this insurance program more affordable to small businesses and their employees.
A small business can purchase this coverage for its employees if it has 50 employees or less and at least 30 percent of the employees earn less than $30,000 per year. Individuals can buy their own coverage if they reside in a household whose income is less than 250 percent of the FPL-just under $42,000. HCRA 2000 sets aside up to $219 million for this program, which will be paid by the state and will not have a fiscal impact on New York City.
Direct Pay HMO Subsidies: Moderate-Income and Above. Currently, all HMOs in New York State are required to offer two mandated HMO plans directly to the general public. Anyone who is not covered by an employer or other group can purchase this insurance if they can afford it. In recent years, the premium rates for these plans have risen significantly-in some cases by over 50 percent. HCRA 2000 attempts to counteract these rising costs by subsidizing a portion of losses incurred by HMOs. Just as in the Healthy New York subsidy, the goal is to reduce the HMO risk by limiting potential losses, which will in turn allow the HMOs to charge lower premium rates. Lower premiums will make direct-pay insurance-which is available to anyone without restriction- affordable to a larger segment of the uninsured population. HCRA 2000 sets aside $130 million of state monies to fully fund this program over three and a half years.
For more information please contact Keith Goldfeld, a senior budget and policy analyst at IBO, at (212) 676-9248.
