In order to control costs and increase quality, New York City created a voluntary Medicaid managed care program in the early 1990s that at its peak enrolled over 400,000 recipients. New York State recently reached an agreement with the federal Health Care Financing Administration that would allow the implementation of a mandatory program for 1.5 million Medicaid recipients in NYC.
Initially, it was envisioned that Medicaid recipients' options would mirror the mix of for-profit and not-for-profit providers in the general managed care market. Over time, however, mainstream commercial plans have left the program and now most Medicaid managed care enrollees are in specialized Medicaid-only, hospital-controlled plans. This article examines the trend toward specialized plans. It then raises questions about possible implications of this trend for some of the program's primary goals, such as providing enhanced competition and choice, improving access to care, and lowering costs.
In New York, as in much of the rest of the country, managed care has been viewed as a solution to two vexing problems that historically have beset the Medicaid program: poor quality and rapidly rising costs. Moving Medicaid recipients into managed care would, in theory, improve access to preventive services that are available to the mainstream insured population. Furthermore, by shifting care from expensive emergency rooms to less costly primary care physician offices, managed care could reduce the cost of the Medicaid program-costs that totaled $13.9 billion in 1999 in New York City.
Initially it was envisioned that the options available to Medicaid recipients would mirror the general managed care market-a combination of for-profit and not-for-profit HMOs that serve the mainstream commercial population. However, because these mainstream plans lack sufficient capacity in low-income neighborhoods to provide adequate access to primary care services, the city and state recognized the need to augment the mainstream plans with a new group of plans that would primarily serve Medicaid enrollees.
These Medicaid-only plans, called Prepaid Health Services Plans, are well positioned to provide the additional capacity because they are predominantly controlled by hospitals that have traditionally served the Medicaid community. In addition to providing more choices, a mix of mainstream and Medicaid-only plans would allow the Medicaid program to benefit from the efficiencies and management experience of mainstream plans while maintaining an important role for traditional Medicaid providers.
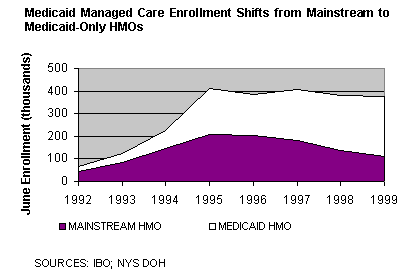
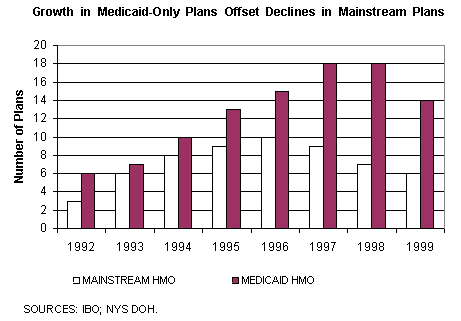
In the early years of the city's voluntary program, mainstream plans-which were attracted by generous reimbursement rates and potential membership-enrolled more than 65 percent of Medicaid managed care members. From 1992 to 1994 enrollment in mainstream and Medicaid-only plans grew at roughly the same rate. Mainstream plans grew from 43,000 to 148,000 Medicaid members, an average annual increase of almost 85 percent. Medicaid-only plans grew by 75 percent annually, from 25,000 to 72,000. The number of plans also increased-mainstream plans from 3 to 8 and Medicaid-only plans from 6 to 10.
The roughly parallel growth ended over the last half of 1994 and the first half of 1995 when enrollment in the Medicaid-only plans grew almost three times faster than in mainstream plans. Several new Medicaid-only plans had entered the market, including one controlled by a majority of the city's academic medical centers. By June 1995, nearly half of 413,000 enrollees were in Medicaid-only plans. By this time, there were 9 mainstream plans and 13 Medicaid-only plans.
In the fall of 1995, amid concerns that managed care plans were using improper marketing tactics, the city and state implemented stricter enrollment policies. These policies effectively halted the growth of the program; between 1995 and 1999 total enrollment remained virtually constant.
Although enrollment was flat during the 1995 to 1999 period, the composition of enrollment was shifting dramatically, with the share of members in Medicaid-only plans increasing to 70 percent. A major factor behind the shift was the state's institution of a competitive bidding process that significantly lowered premium rates. The mainstream plans, which were not dependent on Medicaid revenues, had fewer incentives to remain in the program; many complained that their Medicaid business was not sustainable at the lower rates. Subsequently, almost half of the mainstream plans contracting in the city dropped out and enrollment in these plans declined by 15 percent annually. In contrast, Medicaid-only plans, which rely almost entirely on this program for revenues, were committed to the managed care program. Enrollment in Medicaid-only plans grew at 7 percent a year between June 1995 and June 1999, nearly offsetting the reductions of the mainstream plans.
Outside the Mainstream
Does it matter that the Medicaid managed care industry is different from what was originally intended? An industry dominated by Medicaid-only plans raises questions of financial stability, competition, and choice. With the city is in the midst of a multi-year process to enroll the remaining 1.1 million Medicaid recipients in mandatory managed care plans, it is not yet clear what the impact of the shift will be.
A primary concern with Medicaid-only plans is size. The Medicaid-only organizations tend to be substantially smaller than mainstream HMOs; in June 1999, the average membership of the 14 Medicaid-only plans was under 20,000. Plans with small membership face two main challenges-insurance risk and fixed administrative costs. A smaller plan will feel the impact of a few very sick, high cost members more acutely than a plan with a broader base of healthy members, an issue of particular concern to the hospital-based plans that may attract membership that is generally less healthy. And smaller health plans will have more difficulty offsetting significant fixed administrative costs. If these cost pressures precipitate the closure of some of the Medicaid-only plans, then two goals of the program-providing competition and choice-would be put at risk. One mechanism to relieve the financial pressure would be to raise premium rates, which in turn would limit the ability to achieve Medicaid savings through managed care.
However, there are reasons to be optimistic. Medicaid-only plans understand the needs of this unique population and have access to a broad range of physicians and other providers that know the Medicaid population well and are more likely to be located near where recipients live. Moreover, the long delay in starting the mandatory program may have had a silver lining: the first several years of the program have provided these plans with an opportunity to develop more efficient operations. And finally, some of the issues related to size may be somewhat mitigated by the rapid growth of the program as mandatory enrollment is phased in over the next several years.
For more information contact Keith Goldfeld, a Senior Budget and Policy Analyst, at (212) 676-9248.